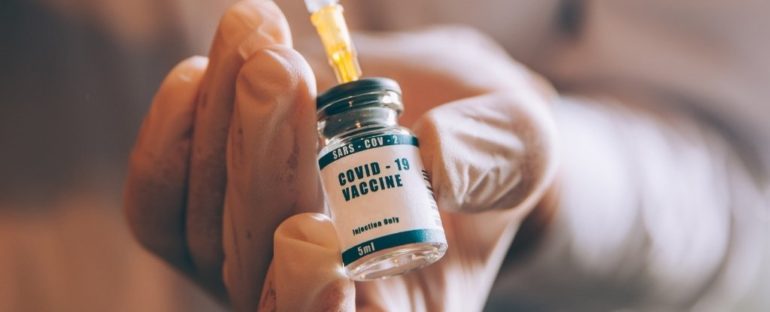
With Pfizer’s coronavirus vaccine being administered across the US and Moderna’s likely to be within weeks, the question of whether to get vaccinated is no longer hypothetical. [Ed. note: The US Food and Drug Administration approved Moderna’s vaccine Friday.]
Federal officials expect that 20 million Americans could be immunized by the end of the year.
By April, vaccines could start being distributed to young, healthy people.
But around four in 10 Americans have said they won’t get a coronavirus vaccine, according to several polls (though some said they might change their minds once more people get vaccinated or more information becomes available).
When it comes to the safety of these vaccines, however, there are good reasons to be confident already. Here are nine explanations to give to a friend or family member who’s sceptical of the shots.
The FDA authorization means expert scientists agree that the benefits of the vaccine outweigh the risks to most Americans.
US hospitals began vaccinating healthcare workers on Monday, just four days after the Food and Drug Administration authorised the vaccine from Pfizer and BioNTech.
The FDA decision was based on the recommendation of an independent panel of scientific experts, who analysed months of data from late-stage clinical trials. Moderna’s coronavirus vaccine will be scrutinised by that same panel on Thursday.
This process is standard for any vaccine, including the flu shots Americans receive every year.
During last week’s advisory panel vote, 17 out of 22 experts agreed that the “benefits of the Pfizer-BioNTech COVID-19 vaccine outweighed its risks for use in individuals 16 years of age and older.”
Four experts voted against that premise, and one expert abstained. These dissenting committee members, for the most part, simply said they wanted more safety data for people ages 16 and 17. One pressed for at least two months of additional data that included more studies of vulnerable groups.
But none cited major safety concerns.
“I would have voted ‘yes’ most enthusiastically had the language been ‘…18 years of age and older,'” Dr. David Kim, who directs the vaccines division at the US Department of Health and Human Services, told Business Insider.
President Donald Trump may have attempted to politicize the vaccine development process, but that didn’t affect the authorization.
Over the summer, President Trump suggested that a coronavirus vaccine may become available “right around” the election on November 3. The comment gave rise to concerns that pharmaceutical companies would feel pressure to rush a vaccine to market.
“I’m rushing it. I am. I’m pushing everybody,” Trump told radio host Geraldo Rivera on August 6.
Soon after, pharmaceutical companies took a rare step to assuage concern: In September, nine leading drug companies, including Pfizer and Moderna, released a joint statement promising to put safety before speed.
The companies vowed to “only submit for approval or emergency use authorization after demonstrating safety and efficacy through a Phase 3 clinical study that is designed and conducted to meet requirements of expert regulatory authorities such as FDA.”
Pfizer also declined US government funds for research and development to avoid potential political conflicts, the New York Times reported. And although the FDA wanted to see infections in at least 64 volunteers in late-stage trials in order to assess a vaccine’s efficacy, Pfizer waited to apply for authorization until 94 people got sick.
Coronavirus vaccines have already been tested in tens of thousands of volunteers, so scientists have a good sense of how people respond.
Study volunteers have been receiving Moderna shots since March and Pfizer shots since April. Both studies are randomised control trials, meaning participants were randomly and blindly assigned to either get the vaccine or a placebo.
Both Pfizer’s and Moderna’s trials are also at or above the average size. A 2012 review found that the average phase-three vaccine trial had around 30,000 participants.
Pfizer’s late-stage trial involved more than 43,000 volunteers across six countries and 16 US states. Eight COVID-19 cases were recorded in the group that got the vaccine, compared to 162 cases in the placebo group. That suggests the vaccine is 95 percent effective in preventing the disease.
Moderna’s trial, meanwhile, involved more than 30,000 participants throughout 30 US states. The researchers observed 90 COVID-19 cases in the placebo group and five in the vaccine group, suggesting the vaccine is 94.5 percent effective.
The most effective vaccine in history, the measles vaccine, is 97 percent effective.
Moderna and BioNTech each designed their vaccines within days, but that doesn’t mean the process was too quick.
Previously, the fastest vaccine ever developed, for mumps, took more than four years.
Unlike traditional shots, however, vaccines that rely on messenger RNA (mRNA) – genetic material instructs cells to make proteins – can be created using just a virus‘ genetic code. Chinese scientists sequenced and published the coronavirus’ genome in January.
“We’re not skipping steps – we actually have better technology,” Albert Rizzo, chief medical officer for the American Lung Association, previously told Business Insider.
“Why did it take two weeks to cross the Atlantic back in the 1800s? Well, we had to go on a boat. Whereas now, you can get across the ocean in several hours.”
BioNTech’s co-founder, Ugur Sahin, made a rough design of the company’s vaccine over one weekend in mid-January, a company spokesperson told Business Insider. Moderna also developed its mRNA vaccine in just two days.
Then Operation Warp Speed helped accelerate Moderna’s process by giving the company $US483 million to develop its shot, $US472 million to advance its clinical trial, and $US1.5 billion in a purchase order for 100 million doses.
Pfizer threw $US2 billion of its own money into its vaccine initiative, the Wall Street Journal reported – including $US500 million for equipment and $US200 million for special machines that encase mRNA in a lipid envelope.
Pfizer tested multiple candidates at once so it wouldn’t have to go back to the drawing board if some proved unsuccessful. It also shaved months off its timeline by making mRNA in disposable bags instead of steel tanks.
Like Moderna, Pfizer manufactured vaccine doses while clinical trials were ongoing. Additionally, the company opted to store multiple doses in a single vial and ship them at subarctic temperatures guaranteed to preserve the shot, rather than test whether doses could survive at higher temperatures.
Vaccines using mRNA technology are relatively new, but scientists have been developing the approach for decades.
Scientists first discovered mRNA in 1961. Roughly 30 years later, researchers at the University of Wisconsin and biotech company Vical Incorporated figured out how to manufacture mRNA so that it would instruct living cells to make specific proteins.
By 2005, biochemist Katalin Karikó – now a senior vice president at BioNTech – had discovered how to configure mRNA to slip past the body’s natural defences to avoid a dangerous immune response.
Her work inspired the founding of Moderna, which focuses solely on mRNA therapies. Before the pandemic, Moderna had entered eight mRNA vaccines into clinical trials, including a flu vaccine.
In 2017, Karikó, along with several other researchers at BioNTech and the University of Pennsylvania, also showed that an mRNA vaccine protected mice and monkeys against the Zika virus. So Karikó said she wasn’t surprised when two mRNA vaccines were found to prevent COVID-19.
“When people are saying, ‘There is no messenger RNA vaccine that’s ever been,’ it is very critical and very important to know that not because it failed,” she told Business Insider. “It just didn’t have time to be advanced by many people.”
An infographic showing how mRNA vaccines are developed. (Shayanne Gal/Insider)
Long-term side effects are unlikely. It’s the short-term ones that scientists typically watch out for — and those generally seem to be mild and fleeting.
Both Moderna and Pfizer followed up with volunteers at least two months after they received their second injection (both vaccines require two doses). No major safety concerns were found.
“Documented adverse effects to vaccines show up mostly in hours, sometimes in days, rarely in weeks,” Megan Ranney, director of the Brown University Lifespan Centre for Digital Health, recently wrote on Twitter.
With mRNA vaccines in particular, the body destroys the molecule fairly quickly, meaning it won’t linger in the body.
Most Pfizer participants reported temporary side effects after being vaccinated, including fatigue, headaches, and pain at the injection site.
People under 55 reported more side effects overall. Among people aged 18 to 55, 4.6 percent reported severe fatigue after getting their second injection, and 3.2 percent had severe headaches.
In Moderna’s trial, nine in 10 people who got the shots registered some side effects, but they were mostly mild or moderate. Around 17 percent reported more serious side effects, including pain or swelling at the injection site, fever, headache, fatigue, nausea, and vomiting.
The side effects typically lasted for one to three days, according to documents released Tuesday by the FDA.
In both trials, these results were consistent across genders, age groups, ethnic and racial groups, and people with preexisting medical problems.
“Prior experience shows that after a vaccine has been approved by the FDA, it is rare to discover any significant new serious unexpected side effects,” Dr. Noam Tau, a physician at Sheba Medical Centre, said in a statement to Business Insider.
Pfizer’s vaccine isn’t yet recommended for certain groups, like pregnant women and young kids, but that’s because of a lack of data – not any known safety problems.
Pfizer tested its vaccine in people ages 12 and older. But the sample size of kids from ages 12 to 15 was too small to weigh the risks, so the FDA only authorised the vaccine for people 16 and up. Moderna, meanwhile, only tested its vaccine in adults ages 18 and older.
Kids are often difficult to include in trials because of ethical and safety concerns. Parents may not feel comfortable signing their kids up to participate, and researchers usually prefer to test vaccines in adolescents before young children.
But there’s little reason to suspect that kids will react poorly.
“Children generally respond well to vaccines,” Donna Farber, a Columbia University immunologist, told Business Insider. “They should respond well or comparably to a young adult – and maybe even better.”
Pregnant women aren’t expected to respond differently, either. Although they have not been included in trials yet, the FDA says pregnant women won’t be denied Pfizer’s shot if they and their doctors decide it’s the right option for them.
Pfizer and Moderna plan to follow up with pregnant women who choose to get vaccinated after the shot is authorised. That’s how public-health experts eventually determined it was safe for pregnant women to get the flu vaccine, even though they were never included in the trials.
FDA reviews have also said there’s “insufficient data” to assess whether the vaccine is safe for immunocompromised people. Though late-stage trials included some people with preexisting health problems, the shot might be less effective if a patient’s immune system isn’t working properly.
Clinical trials have a shameful history among communities of colour, but the recent studies were conducted safely among a diverse group of volunteers.
Many Black Americans remain sceptical of vaccines due to a long history of medical exploitation.
In the 19th century, physician James Marion Sims performed reproductive health experiments on enslaved women without anesthesia. Starting in 1932, the 40-year Tuskegee experiment denied syphilis treatment to Black men who had enrolled under the promise of free medical care.
From 1961 to 1974, the Holmesburg Prison experiment tested toxic substances and mind-altering drugs on Black inmates in Philadelphia.
The recent coronavirus vaccine trials attempted to include a diverse group of participants. Moderna even slowed down its trial in September to allow more time for volunteers of colour to join.
“I would rather we have higher diverse participants and take one extra week,” the company’s CEO Stéphane Bancel told CNBC, adding that diversity “matters more to us than speed.”
As of late October, 37 percent of Moderna trial participants were non-white. Hispanic/Latinx volunteers made up 20 percent of participants, while Black volunteers made up 10 percent and Asian-American volunteers made up 4 percent.
As of Monday, 42 percent of Pfizer’s global trial participants were non-white. Hispanic/Latinx volunteers made up 26 percent of participants, and Black volunteers made up 10 percent. Asian volunteers represented 5 percent of trial participants, while Native American volunteers represented 1.1 percent.
Scientists agree that it’s much safer to get an FDA-authorised vaccine than to risk getting COVID-19, which has known long-term effects.
Many coronavirus patients develop long-term complications from their infections, though researchers still aren’t sure precisely what portion of people experience this.
A July report from the CDC found that about one-third of coronavirus patients surveyed had not recovered after two or three weeks. An August study estimated that one in 10 coronavirus patients experienced prolonged illness.
Many individuals have fought months-long battles with fatigue, muscle aches, trouble breathing, heart palpitations, or difficulty sleeping. Some have reported neurological problems like dizziness, confusion, and delirium. Others have identified strange symptoms like hair loss and red, scaly rashes.
Some COVID-19 patients with long-lasting symptoms also report feeling weak or foggy after too much physical activity – a hallmark of chronic fatigue syndrome, an illness that can last several years or more.
A follow-up study of SARS patients in Hong Kong found that 27% met the clinical criteria for chronic fatigue syndrome four years after their illness began. (SARS and the new coronavirus share about 80 percent of their genetic codes.)
Another study of 109 SARS patients in Toronto found that more than half hadn’t returned to work due to persistent fatigue and weakness a year after they were discharged from the ICU.
“There’s talk in the medical community about a chronic fatigue syndrome-like illness that could happen after coronavirus,” Dr. Nate Favini, the medical lead at Forward, a primary-care practice, told Business Insider.
“Unfortunately, there will be a small subset of people for whom that becomes the case, and these symptoms really do become a chronic thing that you’re dealing with for years.”
This article was originally published by Business Insider.
More from Business Insider: